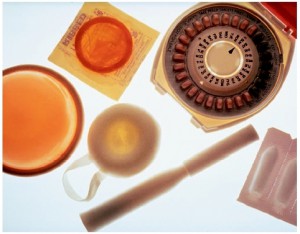
Source: Feministing
Birth control, birth control, birth control.
There’s good reason that it’s a feminist issue, what with the government always trying to have control over our bodies and our fighting back for our right to bodily autonomy.
But as sex educators, something that we’ve noticed is that not everyone really understands their options and how different forms of hormonal birth control work.
Because the truth is: Birth control is not one-size-fits-all. And with all of the choices out there for you, it’s no wonder people get a little bit confused.
And as feminists, we are wholly dedicated to your right to choose.
So if you’ve ever wondered “How the &#%! does this actually work?” or “Which option is best for me and my lifestyle?” then this article is for you.
The Basics
Hormonal birth control works in three ways.
First, it prevents ovulation.
The hormones release consistent doses of estrogen or progesterone (or both) so your ovaries do not release an egg. No egg, no fertilization. No fertilization, no pregnancy.
Second, it thins the lining of the uterus.
The lining of the uterus (or endometrium) thickens throughout your menstrual cycle to prepare for a fertilized egg (or blastocyst) to implant. That implantation, by the way, is the moment at which you become pregnant.
If one doesn’t implant, the lining will shed. Yup. That’s your period. And that’s why your period is an indication that you’re not pregnant: Because if you were, the lining would stay in place to aid in gestation.
The hormones in birth control prevent the lining from thickening, so should fertilization occur, there won’t be a thick enough endometrial layer for it to implant into.
This is also the reason why periods are lighter when taking a hormonal method of birth control.
And finally, it changes the consistency of your cervical mucus (aka discharge). That makes it harder for sperm to travel through the cervix and to an egg.
Phew.
Now that that’s out of the way, what are the different hormonal methods of birth control and how do you choose one?
1. The Pill
The Pill is probably the most well-known method of hormonal contraception.
More often than not, it has a combination of estrogen and progesterone. This is known as the combination pill. If you’re not sure whether or not your birth control pill is a combination pill, it probably is.
But another option is the progesterone-only pill.
This pill, also known as POP-pills or mini pills, contains only progesterone and has a lower dose of hormones overall.
The progesterone-only pill is taking orally every day, at the same time every single day.
The combination pill on the other hand is taken daily (preferably at a similar time every day), and it provides your body with active hormones for three weeks.
The fourth week pills are placebos. They’re sugar pills which contain no active hormones. That’s the week when you will have your period, should you choose to have it.
Thing is: You don’t have to take the placebo pills. They don’t do anything for you, so it’s perfectly okay to just not take them for that week. Or skip them and go right into your next pack of pills without any adverse side effects. After all, the “period” that you experience on birth control isn’t the real thing anyway.
Because your body’s hormones are being controlled by the pills that you’re taking, you’re not experiencing a regular menstrual cycle, which usually has dips and spikes in hormone levels to make your body do different things – like become fertile or get your period.
So if you don’t want to get your period, don’t.
Remember: This is all about choice.
2. The Ring
The ring, or Nuva Ring, is a clear, flexible plastic vaginal ring.
It’s a combination method of birth control, so it has estrogen and progesterone, and the hormones are released by the ring into your vagina and cervix.
The ring is inserted into the vagina once a month for three weeks. On the fourth week, the ring is removed, and this is when your period will come.
But note: Similarly to what we said above, you don’t have to get your period if you don’t want to. It’s up to you. If you decide to skip it, just go straight from one ring to the next.
The ring will sit in your vagina just below your cervix, which is way up in your vagina and serves as the sort of gateway to your uterus. But trust us: If the ring is inserted correctly, you shouldn’t feel it. Kind of like a tampon.
Some people prefer the Nuva Ring to pills because they don’t have to worry about taking a pill every single day. It’s something that you need to remember once a month, rather than once a day.
That being said, some people are not comfortable with a method that requires them to insert an object into their vagina. And that’s okay, too! It’s important that you choose a method that makes sense for you and your life.
It’s important to note that the ring can fall out during penetration. But so long as the ring is washed with warm water (only water!) and reinserted within three hours, you will still be protected against pregnancy.
And hey, since we mentioned it, here’s a little-known tip for you: You should only ever use water to clean anything that goes into your vagina – and that includes when you’re washing!
The pH balance of the vagina is very delicate – anyone who’s ever had a yeast infection can tell you that! – and it’s easy to throw it off.
The secret?
Your vagina is a self-cleaning organ. Kind of like your eyes. And it doesn’t need help getting clean! Most of the things that you do to try to help your vagina – like using soap or douching – actually hinders its natural process of cleaning itself.
Want more information on vaginal health and how to keep it clean and happy? Try this video for starters!
3. The Patch
The patch, or Ortho-Evra, is also a combination hormonal method of birth control.
It is made from sticky, flexible material that sticks to your arm, shoulder, hip, or buttocks (no where else!) and releases hormones through your skin and into the blood stream.
The patch is very sticky and shouldn’t fall off, so you can go on with your day as usual! Yes, you can even swim and shower with it on!
If it does fall off, you have three hours to put on a new patch and still be protected against pregnancy.
The Patch is applied once a week for three weeks. During the fourth week, no patch is applied, and – yup! you guessed it! – you’ll get your period.
4. The Shot
The Shot, or Depo Provera, is a hormonal method of birth control that only contains progesterone.
It is injected into your arm or buttocks every three months, making it a method of birth control that you have to remember very infrequently.
It’s true that some people will have light spotting for a few weeks, but others experience no bleeding at all.
And yes. A lot of people hear “depo” and think weight gain. You can gain weight on Depo. You can also lose weight on Depo. The thing is, Depo is going to change your appetite. Some people feel an increase, while others a decrease. The trick is to be aware of changes occurring and continue your daily routine, which may include eating healthy and exercising.
5. Other Methods
Implants
The implant, or Nexplanon, is a small plastic rod about the size of match that is inserted under the skin of the inside of your arm.
Nexplanon will release progesterone directly into your blood stream and lasts for three years.
IUDs
An IUD, or intra uterine device, is a small, T-shaped device that is inserted into the uterus by a physician. There are two types: hormonal and non-hormonal.
The hormonal IUD, or Mirena, is made from plastic and contains only progesterone. It lasts for five years, and the hormones are released directly into the uterus. Because it’s a hormonal method, most users will experience lighter periods and some will have no period at all after about a year.
The non-hormonal IUD, or Paragard, contains no hormones at all and lasts for up to ten years. It is wrapped in copper, which causes an inflammatory reaction in the uterus, which essentially immobilizes sperm. This method does not contain hormones. As such, you will not experience lighter periods. Rather, it will likely increase the flow of your periods.
Keep in Mind
There are a few things that we want you to remember when choosing a birth control option:
All of the aforementioned methods require either a prescription or insertion by a doctor.
Hormonal methods of birth control, like all medications, are going to have some side effects. Most of these are mild and will go away after a few months. And while serious side effects can occur, these will mostly depend on your past and current medical history, both of which are important for you to discuss with your doctor.
All of these methods come with high effectiveness if you use them correctly. When choosing a birth control method, take into consideration not which method has the highest rate of effectiveness, but which one is going to be most effective for you, your lifestyle, and your relationships.
The first method that you try may not be the best method for you. Sometimes you have to try a couple (or a few!) before you find the best one.
And please remember: None of these methods (none! not one!) will protect you from HIV and other sexually transmitted infections. Please consider using a barrier method in addition to hormonal birth control if this is a concern for you.
***
Deciding to use a hormonal birth control method can be a daunting process, especially if you’re a little confused about how it works (thanks a lot, American sex education!), and it’s okay if you have questions or want advice.
Talking to your doctor is a great first step in figuring out the best birth control method for you.
But if you want to go into that conversation armed with more information, we highly recommend trying My Method by Planned Parenthood. It’s an online app that helps you think about your options.
So go forth now and conquer the world of birth control options!
And should you have any other immediate questions, this comprehensive resource should help.
[do_widget id=‘text-101′]
Blanca Y. Torres is a sexual health educator in the greater Philadelphia area, running community education programs with Latinos and adolescent girls. She is also an Adjunct Professor in Human Sexuality in New Jersey. She holds her M.Ed. in Human Sexuality from Widener University. You can find her on Twitter @blanquitayaneth. She tweets about cheese and sometimes bread.
Melissa A. Fabello, Editor of Everyday Feminism, is a domestic violence prevention and sexuality educator, eating disorder and body image activist, and media literacy vlogger based out of Philadelphia. She enjoys rainy days, Jurassic Park, and the occasional Taylor Swift song and can be found on YouTube and Tumblr. She holds a B.S. in English Education from Boston University and an M.Ed. in Human Sexuality from Widener University. She is currently working on her PhD. She can be reached on Twitter @fyeahmfabello. Read her articles here and book her for speaking engagements here.
Search our 3000+ articles!
Read our articles about:
Our online racial justice training
Used by hundreds of universities, non-profits, and businesses.
Click to learn more




















